This leaflet is to help you understand what atrioventricular-septal-defects is, what tests you need, and the implication of being diagnosed for your baby and your family.
What are Atrioventricular (AV) septal defects?
The normal heart is divided into four chambers: two atria (upper chambers), right and left; and two ventricles (lower cavities), right and left. The two atria are separated by the atrial septum, which presents a small communication that closes after birth during the fetal period. The two ventricles are separated by the interventricular septum. Two valves allow blood to pass from the atria to the ventricles and not return backwards. There is one on the right side and the other on the left side.
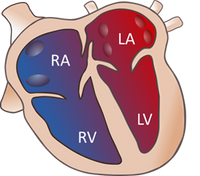
Normal Heart
Atrioventricular septal defects are congenital heart diseases characterized by a defect or hole in the interatrial septum and interventricular septum, with a single valve for the right and left side of the heart or a valve that is partially separated. There are three types of septal defects depending on the degree of alteration:
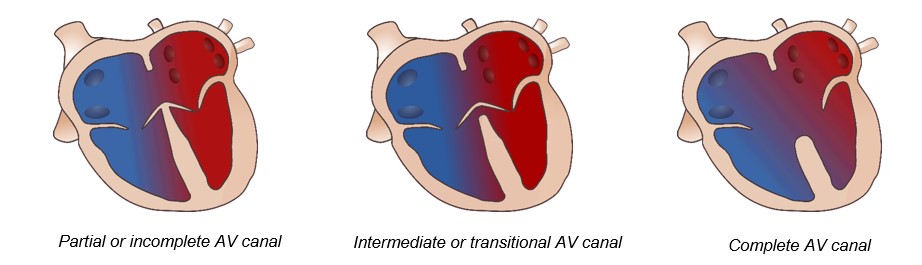
How does an AV septal defect happen?
In fetal life, there is a defect in the development and connection of the atrioventricular valves with the cardiac septum (septum between the two atria and the two ventricles). Multiple factors may cause this cardiac defect; there is a strong association with genetic abnormalities, especially Down syndrome.
Why is AV septal defect important?
AV septal defect can be associated with important anomalies in the heart and, in up to one-third of cases, abnormalities in other body parts.
In addition, it is associated, in up to half of the cases, with chromosomal and genetic abnormalities, of which the most frequent association is Down syndrome.
In most cases, gestation reaches the end of the pregnancy without incident. However, cases with significant valvular abnormalities or irregular heartbeats (cardiac arrhythmias) may develop fetal heart failure with the risk of intrauterine death.
What are the things to watch for during the pregnancy? Should I have more tests done?
Prenatal diagnosis of an AV canal involves a detailed fetal ultrasound and an advanced echocardiography (a specialized ultrasound of the baby's heart during pregnancy) to rule out other associated heart defects or anomalies in other body parts. Parents should be offered an invasive technique to rule out associated chromosomal or genetic abnormalities.
Monthly ultrasound monitoring is recommended to rule out signs of fetal complication: fetal heart failure (if valvular insufficiency is present) or an arrhythmia (AV block). In addition, all cardiovascular structures should be evaluated at each scan.
Where should I deliver? Where will the baby receive the best care after it is born?
Although most newborns with an uncomplicated AV canal do not usually present problems in the first days after birth, delivery at a tertiary level hospital is recommended.
What does it mean for my baby after it is born?
Once the child is born, as a result of the abnormal communication between the two sides of the heart, blood from both sides mix, and too much blood re-circulates back to the lungs instead of back to the body. This means that the heart works harder than it should and will become enlarged and damaged if the problems are not repaired/solved.
The clinical features of heart failure begin within the first months of life, except in some cases with other associated heart defects or an atrioventricular valve insufficiency, which may appear earlier. Symptoms of heart failure in infants include feeding difficulties, drowsiness, lethargy and failure to thrive.
AV canal treatment is surgical. Surgery is performed in the first year of life and earlier than 3-6 months in patients with more symptoms.
Will it happen again?
In the case of a previously affected child, the risk of having another child with the same pathology is 2-3%.
